 March 1, 2016
March 1, 2016
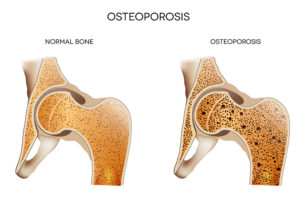
According to the Mayo Clinic, Osteoporosis a condition in which the bones become brittle and weak, with the resulting weakening leading to an increased potential for broken bones, fractures, and general muscular-skeletal concerns. Since Osteoporosis occurs mainly in older individuals – especially Asian or Caucasian woman who are beyond menopause, it can be especially debilitating and harmful when paired with other old-age risk factors. For instance, poor vision or depth perception can cause a trip or fall, and Osteoporosis can then cause the seemingly innocuous fall to result in a broken wrist or hip. Older individuals must be vigilant and highly aware of the warning signs of Osteoporosis, as well as the treatment methods that have proven effective at combating this debilitating affliction.
Screening for Osteoporosis
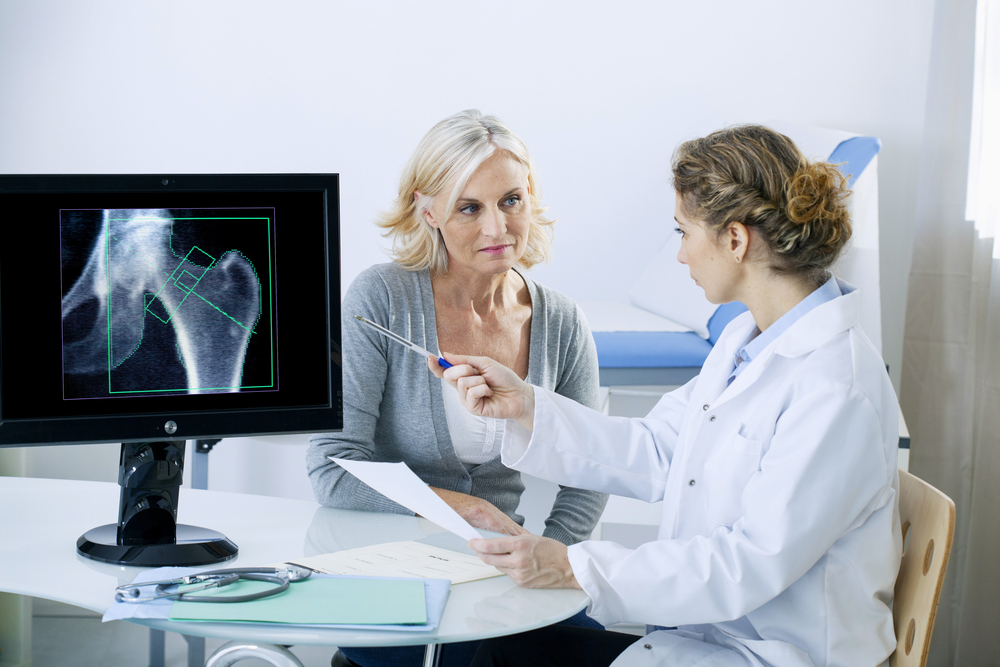
Recognizing the early symptoms of this condition is crucial to preventing further bone loss throughout the upcoming years. While some side effects are easy to spot early on, others are quite invisible unless the patient is examined by a qualified healthcare professional. Instead of waiting until symptoms are obvious, step one in effectively detecting osteoporosis is to visit the doctor.
- Get screened – According to recent studies, findings show that only about 12% of individuals with Osteoporosis actually undergo a bone mineral density screening, or BMD. This is shocking when you consider that the BMD test is generally considered as the most reliable way to uncover actual Osteoporosis in patients. A specialist will conduct a screening panel that is referred to as DXA or DEXA – dual x-ray absorptiometry. This test serves to uncover the actual density of the bones in the patient’s body, and it uses extremely low levels of radiation to do so.
- Identify if you’re at general risk – If you are a woman over 65 years of age, have a family history of Osteoporosis or low body weight, or have had a fracture or broken bone as a postmenopausal woman, you would generally be considered as an at-risk patient. Make sure that you sign up for a BMD test early on, as it is nearly impossible to “feel” if you are losing bone density. It can happen over time, without any real notice or trigger, and symptoms may not show up until years after the bone loss began.
Symptoms that may indicate Osteoporosis
Even if you’re scheduled for a doctor’s visit to test for Osteoporosis, you’ll want to continue to observe your body, or the health and wellness of your loved one, for outright signs of the disease. The following list contains several of the most common conditions that can lead to an Osteoporosis diagnosis:
- Vitamin D deficiency
- Aching joints or muscles
- Loss of height
- Problems getting into or out of chairs without using upper body or arm strength
- Elevated levels of alkaline phosphate or serum calcium during routine blood tests
- A resting pulse that registers more than 80 beats per minute
- A noticeable or worsening curvature of the spine
Complications from Osteoporosis
Though Osteoporosis can be managed with treatment, there are a host of side effects that accompany this condition. Many patients will experience unbelievable pain in their back – sometimes caused by actual fractures in the vertebrae. These fractures can lead to mobility concerns and disfigurement. Compounding the root cause of the back pain, limited mobility can interfere with a patient’s ability to recover and rebuild healthy bones in the back.
Patients will also notice a greater likelihood of bone fractures – and these fractures can take significantly longer to heal that would be expected in a healthier individual. Persistent and lasting pain can interfere with the individual’s mental well being, and a sense of loneliness or a tendency to withdraw from social situations may occur. After all, the afflicted individual may be less able to participate in family outings or even moderately strenuous activities, leading to a feeling of distance.
Treatment Options for Osteoporosis
Luckily, Osteoporosis can be reversed and minimized by applying several treatment principles. Patients should consult their healthcare provider to create a specialized treatment plan, but the following are commonly accepted ways to minimize bone loss, reduce the chance for fractures, and manage pain:
- Prescription drugs can help to treat the condition, and can reduce pain in the process.
- Early lifestyle changes can help to minimize the chances that Osteopenia (a mild form of Osteoporosis) will transition into full-blown bone density concerns.
- A new fitness program including moderate weight-bearing exercises.
- Strontium treatment may be an option that can help to reverse bone thinning.
- SERM treatments can help to reduce bone loss in post-menopausal women.
Osteoporosis is, in most cases, a manageable condition for most patients. Whether you provide care for an individual of advanced age or you’re concerned about bone loss yourself, take the time to schedule an appointment for a bone density test soon – your future self will thank you!
Need compassionate in home care? We can help.



